Chronic Otitis/Chronic Ear Infection in Dogs
Updated on May 01, 2024

Chronic otitis is basically a long-lasting ear infection that can affect any dog, causing itchy, painful, smelly ears. Quite a few things can cause the disease — parasites, allergies, growths — which is progressive and can lead to a rupturing of the eardrum or narrowing of the ear canal.
Treatment starts with cleaning the ear and using medications such as antimicrobials and anti-inflammatories, but in some cases surgery is the best option.
All featured products are chosen at the discretion of the Vetstreet editorial team and do not reflect a direct endorsement by the author. However, Vetstreet may make a small affiliate commission if you click through and make a purchase.
What are Chronic Ear Infections In Dogs?
Chronic otitis is a common disease of the ear canal of dogs. Otitis can be externa (of the outer ear canal alone), media (involving the middle ear), or interna (involving the inner ear and associated structures).
Unlike the typical ear infections humans suffer (children, especially) in which the middle ear is typically affected, this disease is one that affects the external ear canal primarily and the middle and inner ear secondarily. As such, this disease in dogs is categorized as a dermatologic (skin-related) condition.
The typical disease process is as follows: Irritation to the skin lining the ear canal causes inflammation, which results in excess wax production and a comfortable environment for yeast and bacteria (normal residents of the ear canal) to overgrow.
These microbes cause significant itchiness and more inflammation, which leads to an itch-scratch cycle conducive to self-trauma via headshaking, pawing, and rubbing of the ears.
Any dog can develop an ear infection regardless of ear shape, exposure to water (swimming), or the amount of hair inside the ear canal. That’s because the underlying cause of the irritation that initiates the disease process is typically allergic or otherwise unrelated to conformation and moisture.
Environmental allergies (atopy) and food allergies can cause allergic skin disease, which is a common reason for otitis externa. Allergic skin disease may also be influenced by the presence of thyroid disease or adrenal gland disease (Cushing’s disease).
Other less common causes of otitis externa in dogs include:
- Polyps or other growths in the ear canal
- Foreign bodies in the ears, including dirt, sand, or plant material (foxtails and grass awns)
- External parasites (like ear mites)
The most severely affected patients often get stuck in a cycle of inflammation, infection, and thickening of the tissues lining the ear canal (fibrosis), which eventually leads to narrowing of the ear canals, ruptured eardrums, and debris and infection within the middle ear — a highly painful process, to be sure.
Over time, scar tissue occludes the canals, preventing medications from reaching the diseased portions of the canal. The occluded canals also prevent the natural sloughing of the canal’s skin cells, sebum (wax), and hair, which accumulates in both the canal and middle ear, thereby intensifying the infection.
Considering the long-term nature of this condition, chronic otitis is a frustrating disease for both owners and veterinarians. But for patients, the disease is much more critical, given that they typically suffer significant pain. The pain — not to mention the nagging itchiness — associated with these ear infections makes our frustration seem petty in comparison.

Signs and Identification of Canine Ear Infections
Affected dogs typically experience recurrent bouts of malodorous discharge, moderate pain, and terrific itchiness. But a significant subset will suffer these symptoms on a constant basis with no respite from their profound discomfort. Some pets may even try to bite someone who attempts to touch their ears or head.
The clinical signs of otitis (chronic ear infections in dogs) depend on the severity of the inflammation but may include:
- Shaking the head or rubbing the head and ears on the floor or furniture
- Scratching at the ears
- Discharge from the ears, which can sometimes have a foul odor
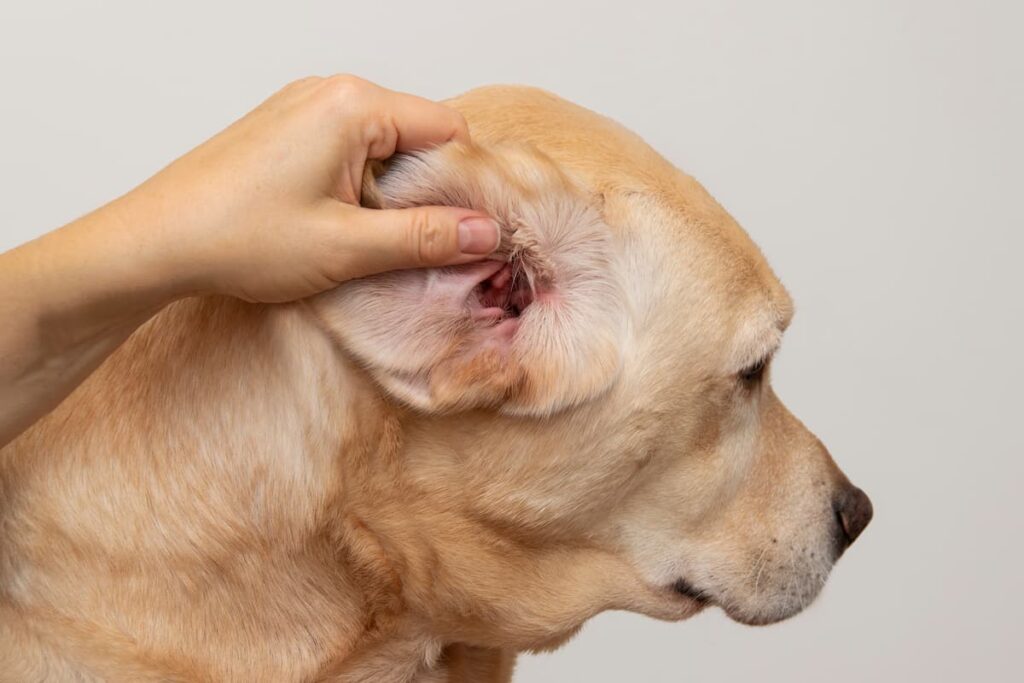
- Redness of the ear canal and earflap (the ears may also feel warm when touched)
- Ear hematoma, evidenced by a grossly swollen earflap
- Aggression whenever the head is approached
Some dogs with severe otitis may cry or groan as they rub and scratch their ears. Others will scratch so severely that their nails create wounds on the skin around their face, neck, and ears. If the otitis is severe or chronic, the outer ear canal can begin to thicken and become deformed.
This thickening can make the ear opening very narrow, so cleaning the ears becomes more difficult. Ulcerations on the inside of the ear canal can also result from infection and self-trauma.
As mentioned above, chronic otitis that begins in the outer ear canal can ultimately rupture the eardrum, ending in otitis media and otitis interna.
Progression of this infection into the middle and inner ear can be associated with even more severe clinical signs, including development of a head tilt, incoordination, inability to stand or walk, hearing loss, and severe, unrelenting pain.
A medical history and physical examination findings can provide valuable information for your veterinarian when trying to diagnose an ear infection. The medical history may include trying to determine how long the ear infection has been going on, whether it has occurred before and whether any other signs of illness have been observed.
Physical examination findings may reveal evidence of underlying illness, such as thyroid disease and Cushing’s disease.
Diagnosis of chronic otitis is usually based on a history of previous ear infections and physical examination findings. Redness, inflammation, discharge, and other changes within the ear will readily indicate the presence of an ear infection. That’s the easy part.
The hard part is finding out a) what kinds of microorganisms are taking advantage of the dog’s inflamed ears and b) what’s causing the inflammation in the first place.
Testing for Chronic Otitis in Dogs
Determining both a) and b) generally requires diagnostic testing. In the case of identifying microorganisms, these are the tests most commonly used:
Microscopy: The most common test used to identify the presence of mites, bacteria, and yeast is a simple evaluation of the discharge obtained from the ear under a microscope. Mites are readily identified in this way. With special staining techniques, yeast and bacteria can also be identified and their characteristics evaluated.
Culture and sensitivity testing: Testing the debris inside a dog’s ear using simple microscopy isn’t always enough when the otitis has been stubborn or severe. Obtaining a sample of the discharge using a sterile swab and submitting it to a diagnostic laboratory will help determine exactly which bacteria and/or yeast are present. This information helps veterinarians devise the ideal drug strategy to treat the infection.
Underlying illnesses leading to the overgrowth of microorganisms will require a different approach. Here are the most common tests:
Otoscopy: An otoscope is a tool used to help a veterinarian visualize the ear canal. This is the ideal tool to help identify the presence of an eardrum rupture, a polyp, or a mass in the ear canal. Unfortunately, most dogs require sedation — if not anesthesia — before they’ll submit to this kind of examination.
Thyroid testing: To determine whether thyroid disease may be playing a role.
Adrenal gland testing: Tests to explore the possibility of Cushing’s disease are sometimes required in dogs with otitis externa.
Allergy testing: Testing for allergies is never embarked upon lightly, but it’s something owners of dogs with otitis externa may have to consider.
Food trial: Since food allergies are such a common feature in the chronic otitis landscape, food trials are perhaps even more important than blood testing. Most food allergic dogs are allergic to the primary protein source in their food.
A food trial’s goal is to change the proteins the patient eats to those she’s never been exposed to before. If the otitis resolves when the diet is changed, a food allergy may be the underlying cause of the condition. A 12- to 16-week period in which the diet is restricted is considered the ideal approach to undertaking food trials.
Affected Breeds of Ear Infections
Breeds of dogs predisposed to allergic skin disease are also predisposed to chronic otitis externa. Breeds with floppy ears or hairy ears, such as Basset Hounds, Labradoodles, Beagles, Golden Retrievers, Labrador Retrievers, and Cocker Spaniels, can be more susceptible to ear infections.
Treatment for Chronic Otitis in Dogs
Treatment of chronic otitis (chronic ear infections in dogs) is a multistep process. First, the bacterial and fungal (yeast) component must be addressed along with the inflammation. The following strategies are typically used:
- Cleansing the ear canal is always recommended to clear accumulated debris. This can be done at home with a soothing cleansing solution like Silver Honey® Rapid Ear Care Vet Strength Ear Rinse, which helps loosen and remove debris, dirt, and wax build-up in your dog’s ears that could cause infection. If the otitis is painful and/or an extensive process, cleansing should ideally be undertaken by a veterinarian with the pet under sedation or anesthesia. Otoscopy is often recommended as an aid in this process.
- Topical medication tailored to treat the specific bacteria, yeast, or mites present is typically used (these are usually available as either ear drops or ointments). These include antibiotics, antifungals (to kill yeast), anti-inflammatory drugs (like cortisone), and topical anesthetics.
- Systemic antimicrobials (antibiotic given by mouth or injection) are indicated in some cases, such as if the eardrum is ruptured. Ideally, antibiotic therapy is based on the results of culture and sensitivity testing.
- Systemic anti-inflammatory medications, such as corticosteroids, are sometimes employed to reduce the pain, redness, and swelling. Antihistamines may also be prescribed.
Treatment of the underlying illness is needed to halt this disease. Treatment will depend on the underlying cause but can range anywhere from mass removal and mite killers to diet changes and allergy injections.
Unfortunately, surgical intervention is sometimes required in stubborn cases where patients suffer stubborn or advanced versions of the disease.
The Importance of Dog Health Insurance
Dog health insurance can help you pay for unexpected health expenses, surgeries, or medications of senior dogs. It’s important to purchase insurance before there’s a problem. While pet insurance may add to your monthly expenses, it can save you hundreds or thousands of dollars in the long run.
Don’t ever let financial decisions get in the way of your dog’s care. Review personalized options for your pet below:
Prevention of Chronic Ear Infections
There is no known means of prevention for chronic otitis. Because it’s assumed there’s a hereditary predisposition for allergic skin disease, thyroid disease, and Cushing’s disease, there are few preventive measures dog owners can take on this front. Careful cleaning and assiduous management of the ear canals is not enough for most patients. But regular cleaning and veterinary checkups can help catch “flare-ups” before they progress.
This article has been reviewed by a Veterinarian.


